MEND
Healthcare · Web app
Client
Duration
Penn Medicine Center for Health Care Innovation and Department of Psychiatry
5 months
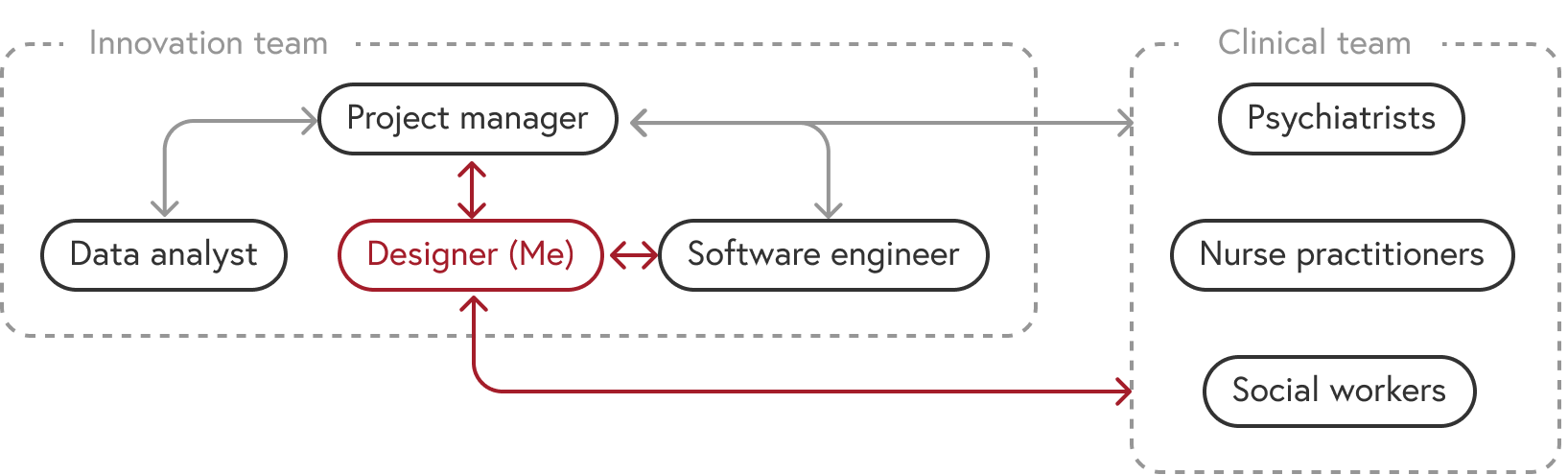
Primary Responsibilities
Team
Improve the workflow of psychiatry clinical providers, focusing on their task of data entry through a web dashboard

Overview
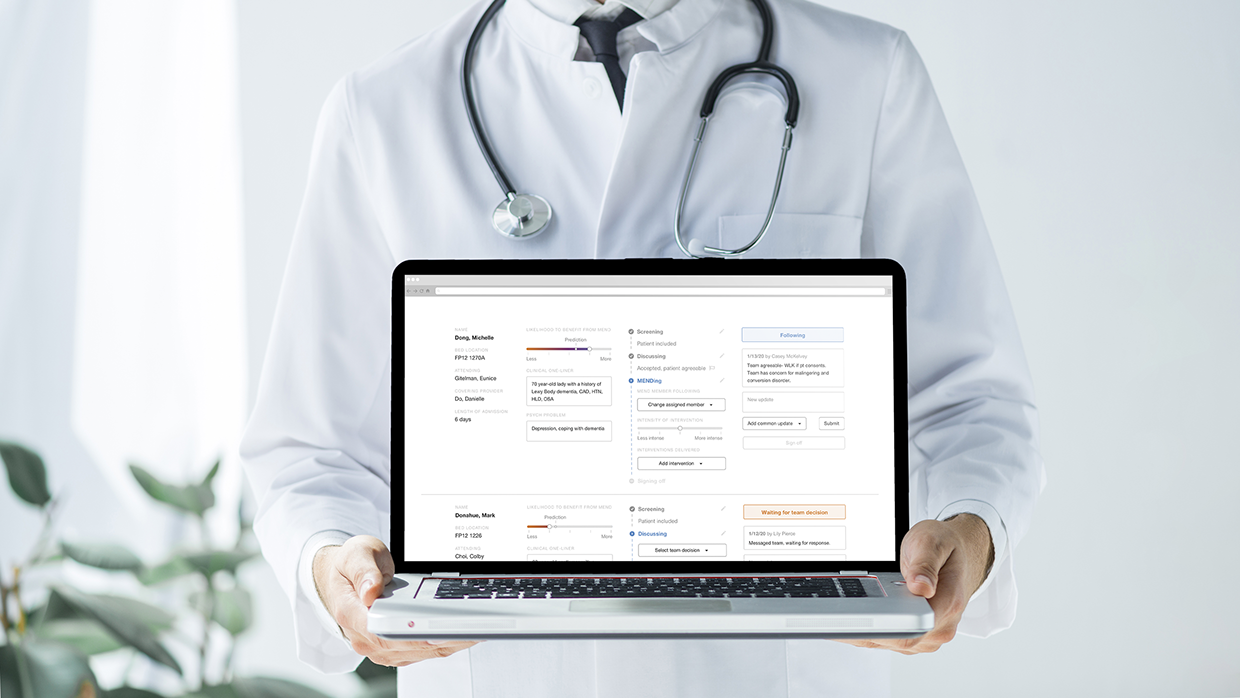
I re-designed a web dashboard used by psychiatry medical providers to reduce the burdens they experience during data entry.
Introduction
Patients admitted into the hospital often experience a broad array of mental health challenges, but a lot of them never receive the psychiatry intervention they need, until the episodes become too acute to be neglected.
MEND (Mental health Engagement, Navigation and Delivery) is a psychiatry service program that aims to proactively provide mental health support to patients.

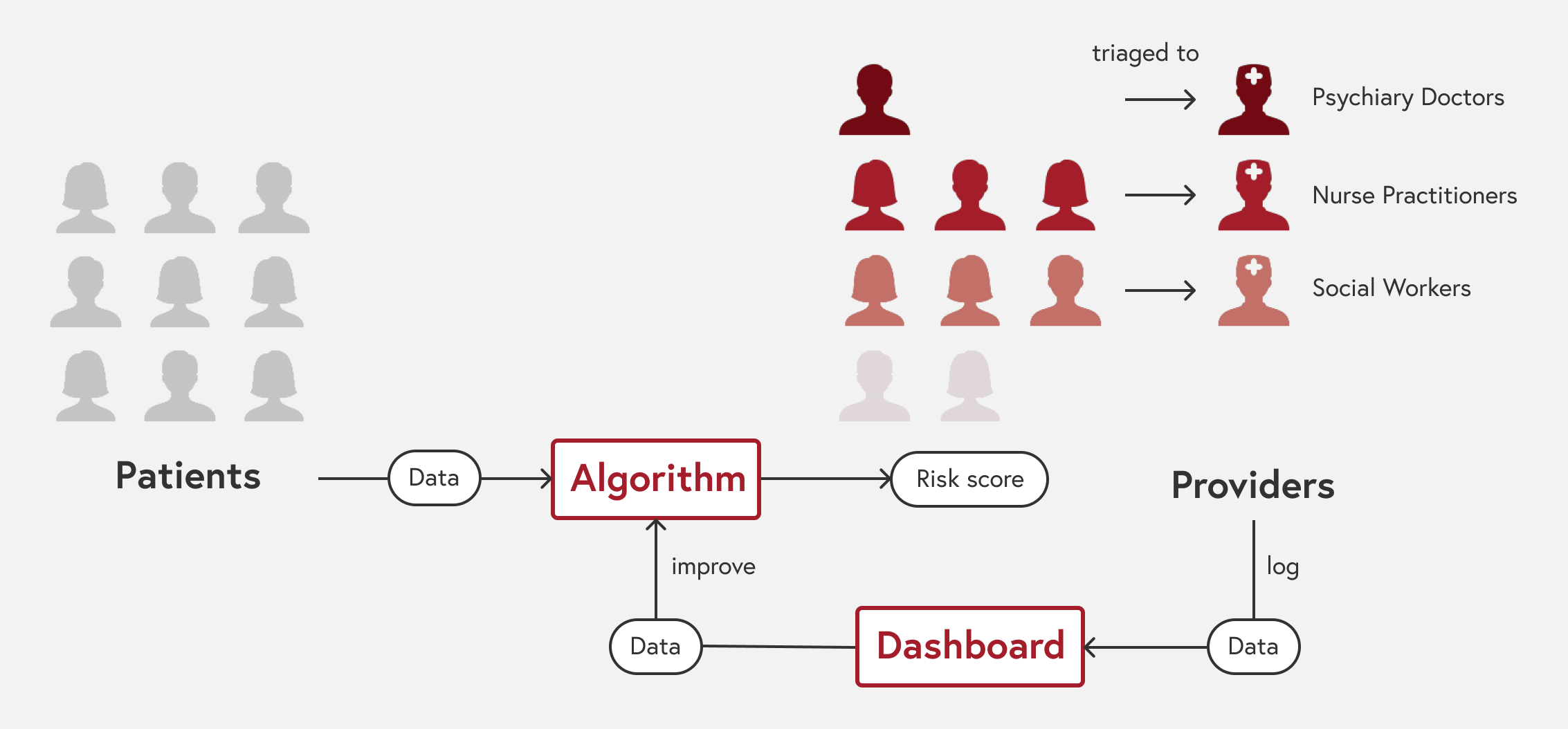
Using patient data from EMR, an algorithm generates risk scores. Based on these, patients are triaged to different levels of providers (e.g. the more severe cases will be intervened by medical doctors).
The providers will also log their interventions through a dashboard, and these data will be used to further improve the algorithm to predict better risk scores. This part is the focus of my project.
Challenge
Initially, when reviewing the logged data of MEND service results, 22% of the cases were never documented through the dashboard. This would lead to the loss of important data that are beneficial for improving the service and its algorithm.
Based on this, our team formed the following design challenge statement:

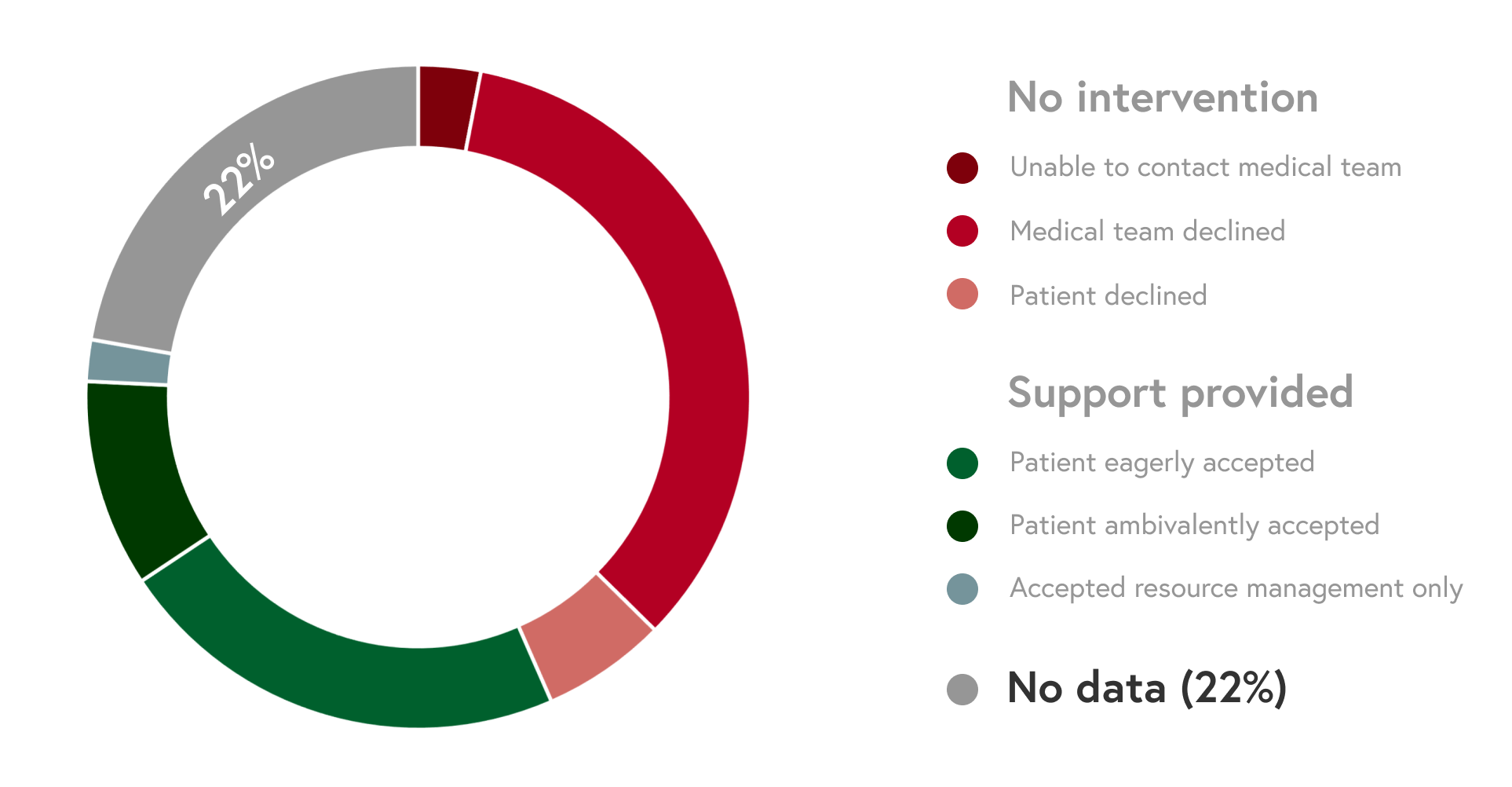
How might we reduce the burdens that MEND service providers experience during data entry so that we can capture a more complete picture of MEND services delivered?
Research Methods
01
Shadowing

Activities
I followed MEND providers throughout the day to observe how they deliver the service.
Rationale
I chose this method as the first activity, assuming it will allow me to obtain the richest contextual information and help me understand the problem space fastest.
Dr. Anderson (MD, middle) and Colleen (CRNP, right) were two of the MEND providers that I shadowed.
02
Journey mapping

Activities
I used notes from shadowing to create a journey map of MEND providers, looking at their interactions with each other, the documentation tools they used, etc.
Rationale
I chose this method to analyze the end-to-end user journey, with a goal to identify patterns, gaps, and opportunity areas.
03
Visual discourse analysis
A stack of the paper patient spreadsheets.
Activities
During shadowing, I discovered that MEND providers print and carry a patient spreadsheet every day. I collected these paper spreadsheets and analyzed what they write, mark, and draw on the paper.
Rationale
I want to study how they parse and document information, which information are more important to them, and how this physical artifact co-exists with digital tools, including the dashboard.
04
Interviews and usability testing

Artifact from user testing (more info about this later)
Activities
I conducted semi-structured interviews in the MEND providers' offices, inquiring about about their experiences with the dashboard and doing usability testing by asking them to complete tasks on the dashboard while observing their interactions.
Rationale
I chose this method to analyze their specific interactions with the dashboard.
Result

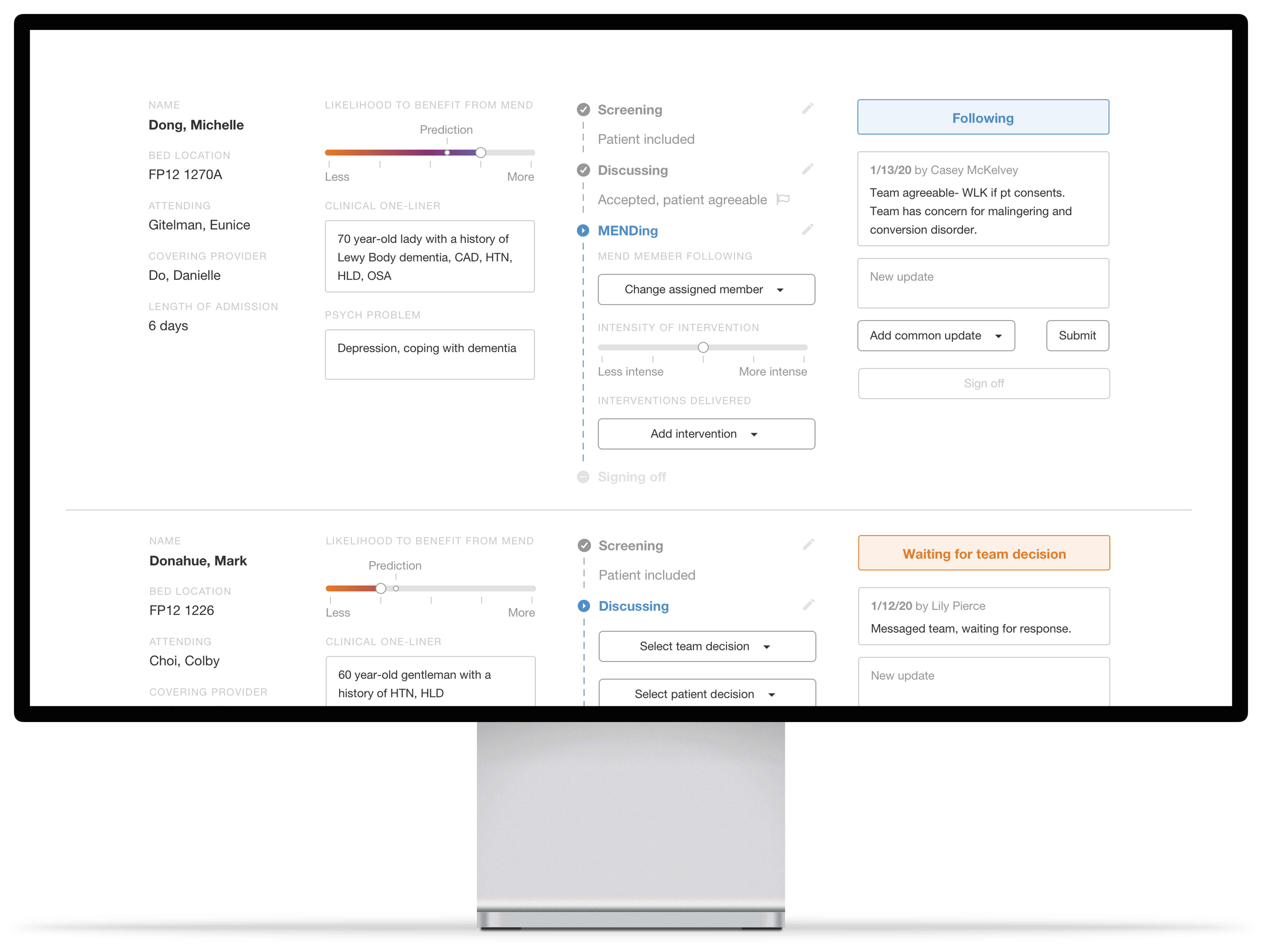
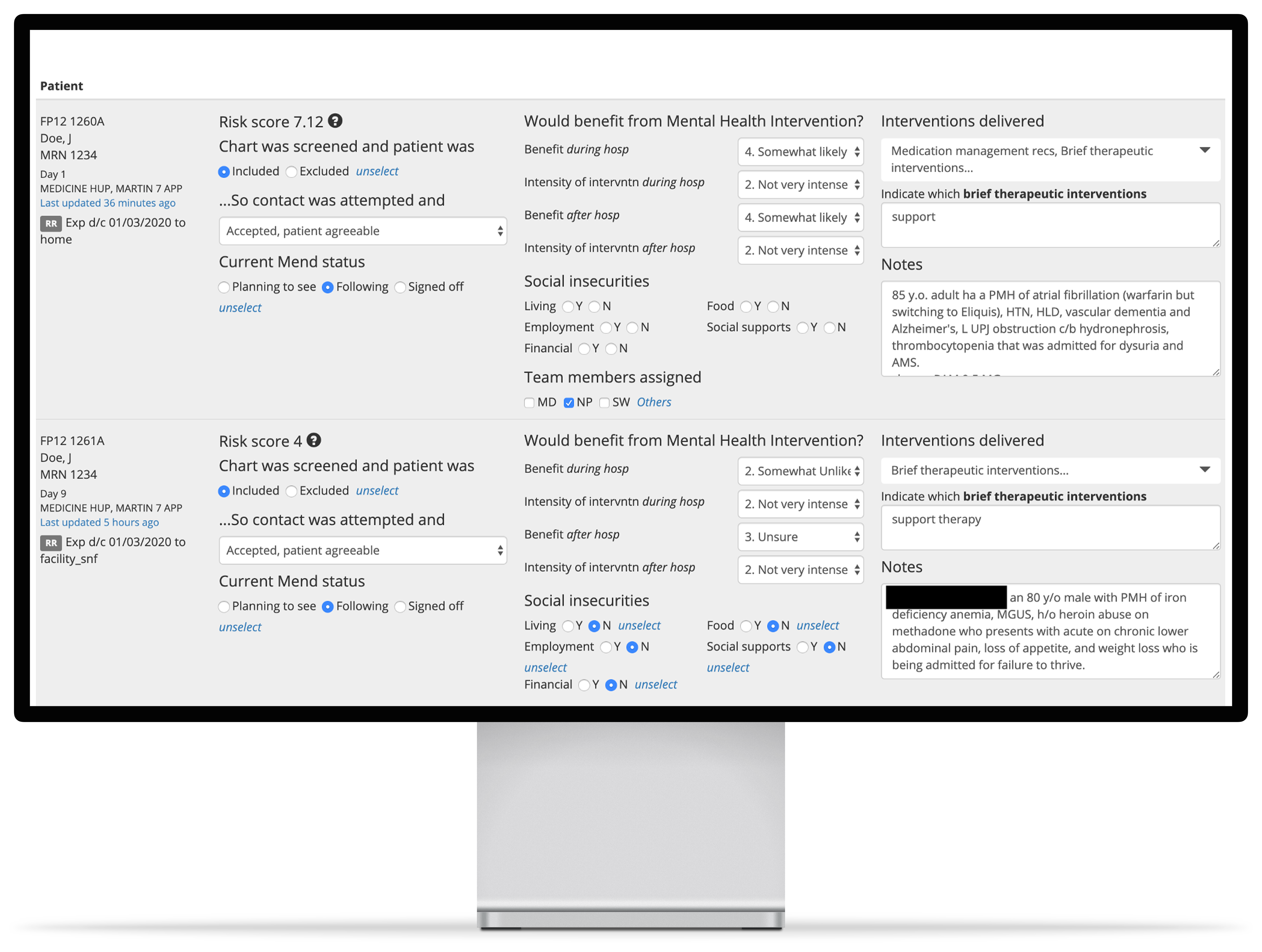
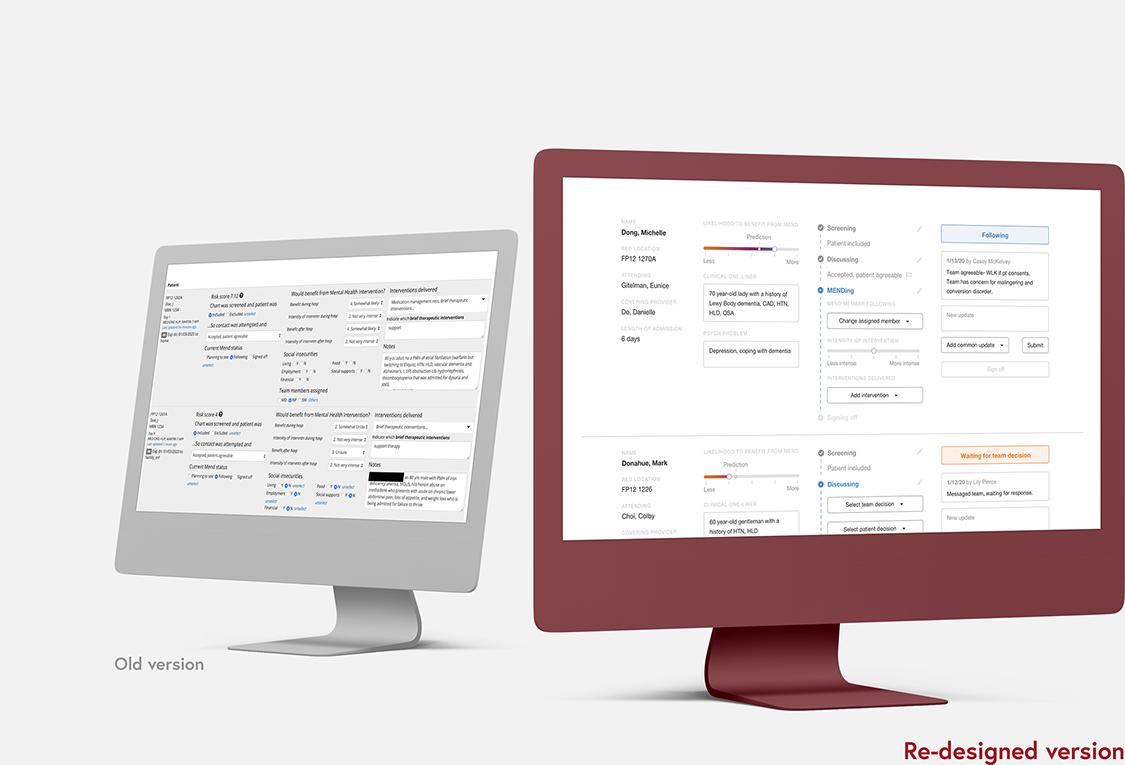
Before-and-after comparison of the dashboard (move cursor to adjust the split)
Below, I want to share two of the design decisions I made.
01
New layout of information and input fields
Insight from research

The old layout of the dashboard was illogical,
leading to a disorganized flow of interactions.
Logic flow of the old design
Artifact from user interview with one of the providers
When shadowing MEND clinical providers, as they used the dashboard to screen patients, I noticed how their cursor would move all over the computer screen across different items.
For data triangulation, I printed out the dashboard on paper and asked a provider to draw her interaction flow of using the dashboard in steps. As expected, the provider ended up drawing messy arrows across the interface, confirming my hypothesis that the interaction flow is disorganized.

I further hypothesized that this flawed flow might ultimately result in users spending more time navigating through information and neglecting certain input fields, which would account for the 22% uncompleted patient cases.
Design action
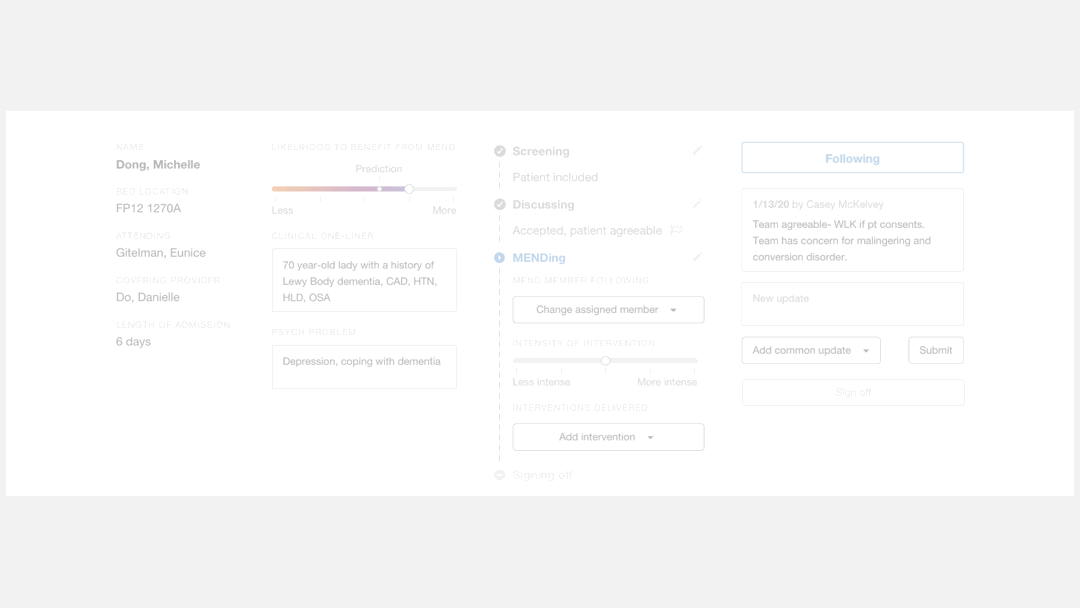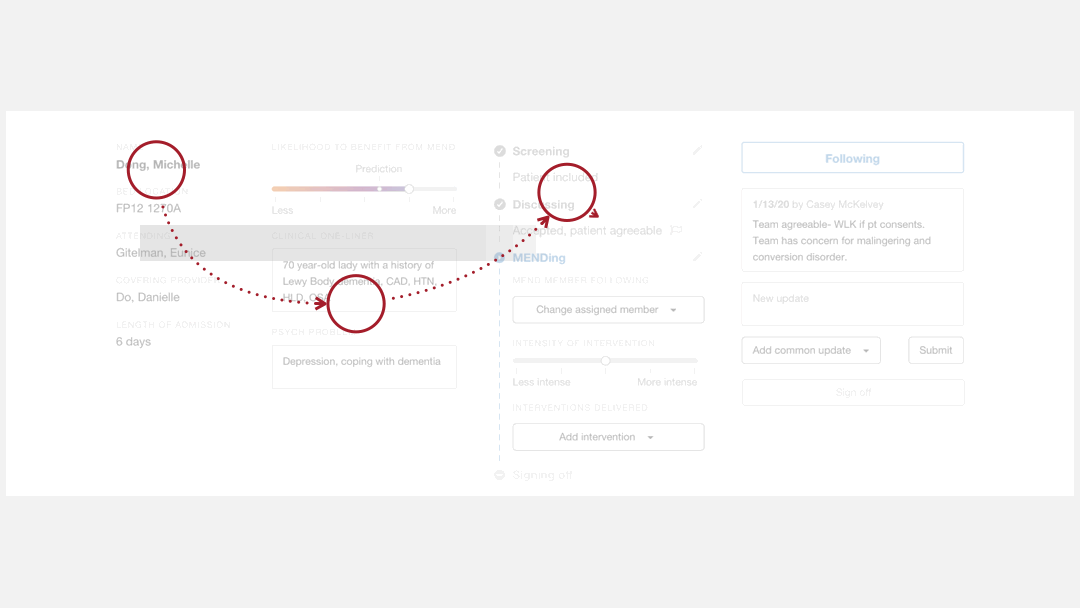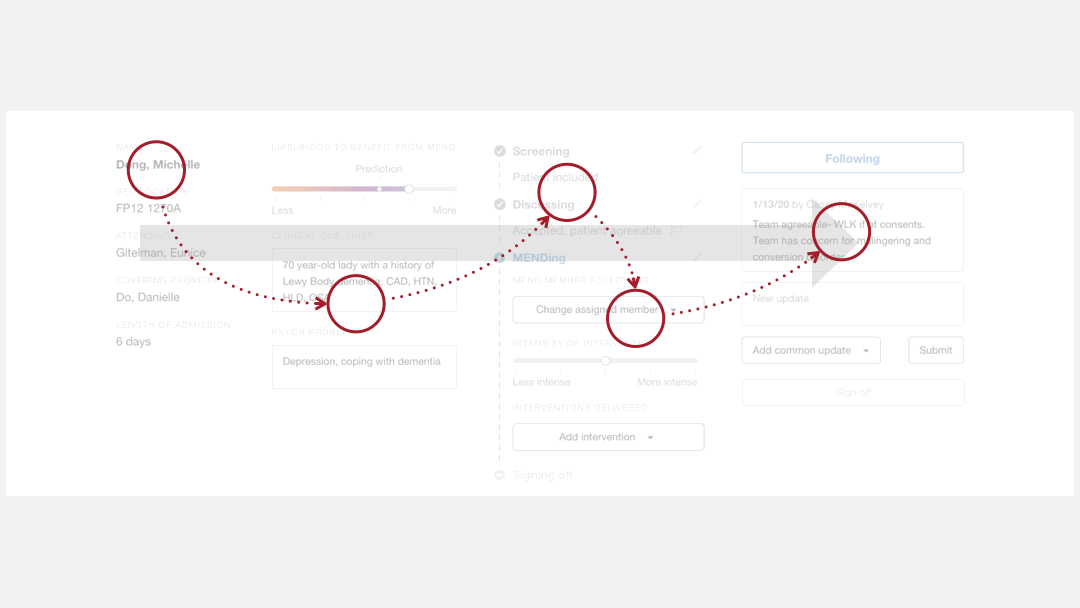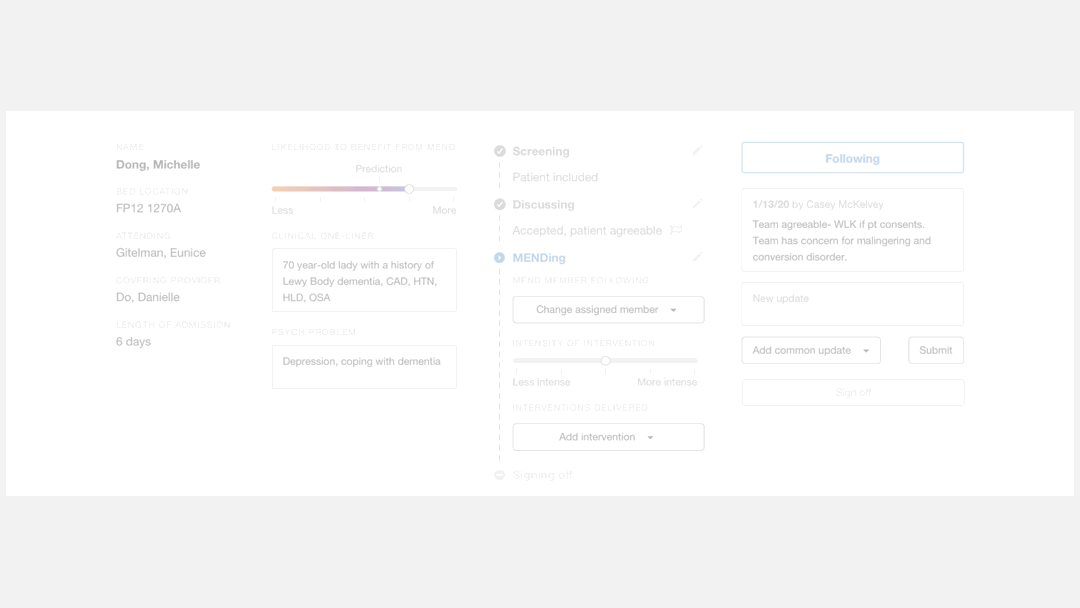
I re-organized the dashboard elements to fit the
logic flow of the providers when they use it.
Logic flow of the new design
I moved information items and data input fields according to the providers’ workflow that I observed through research. These elements were rearranged so that providers could navigate through them in a top-to-bottom, left-to-right fashion, which is a natural reading pattern for humans.
Desired outcome
My assumption was that by changing the layout, the users could spend less time documenting on the dashboard without neglecting any input fields.
02
New "Updates" section
Insight from research
The MEND provider team works in a highly collaborative manner.
Patient cases could be handled by multiple providers on the MEND team throughout the time that the patient is in the hospital. Each day, MEND providers will write down who is responsible for which patient case on the printed patient list that they carry around.

Provider's notes on who is responsible for which patient
(SW - social worker, NP - nurse, MD - physician)
As a result, collaborating and communicating updates about patient cases has been an integral part of their workflow. Because of this, the MEND provider team wants dashboard features to help with these collaboration. During a focus group interview, one of the providers requested features to help distinguish between notes authors:
“Can we have color variation for team members [so we know who wrote which patient case update]?”
However, the old dashboard had underwhelming
features that would make collaborations easier.

Old interaction of documenting an update
The “Notes” section where providers wrote updates on patient cases was just a free-form text box. To view and write new updates, which is a frequent user action, the provider needed to scroll down within the text box, because the first few lines in the text box were usually clinical info about the patient.
My hypothesis was that this increased the time providers spent to review patient cases.
Design action
I designed an “Updates” section for the providers to write and view updates of patient cases easily.
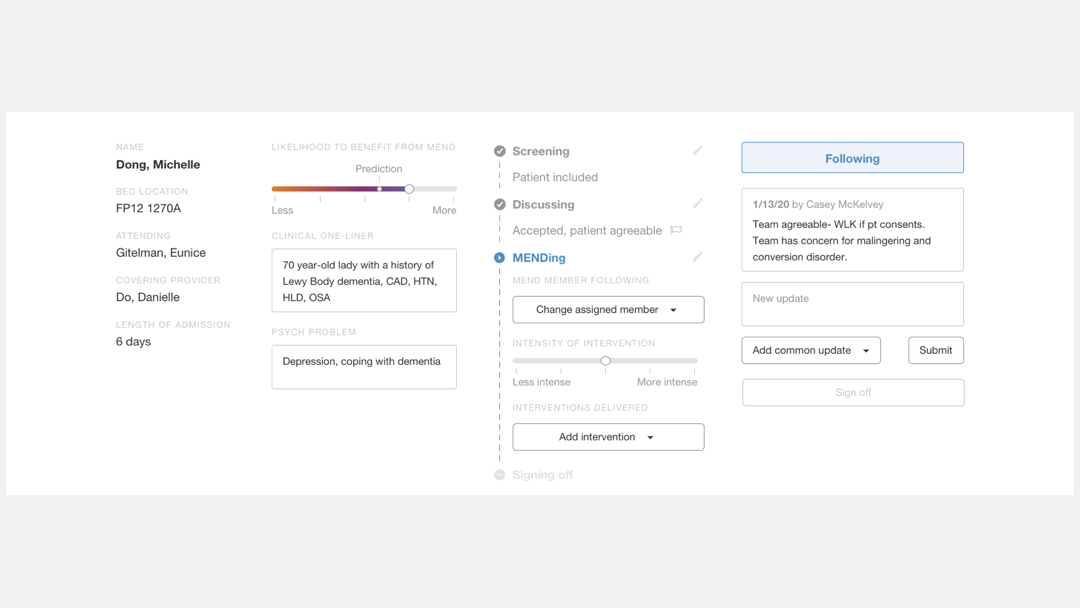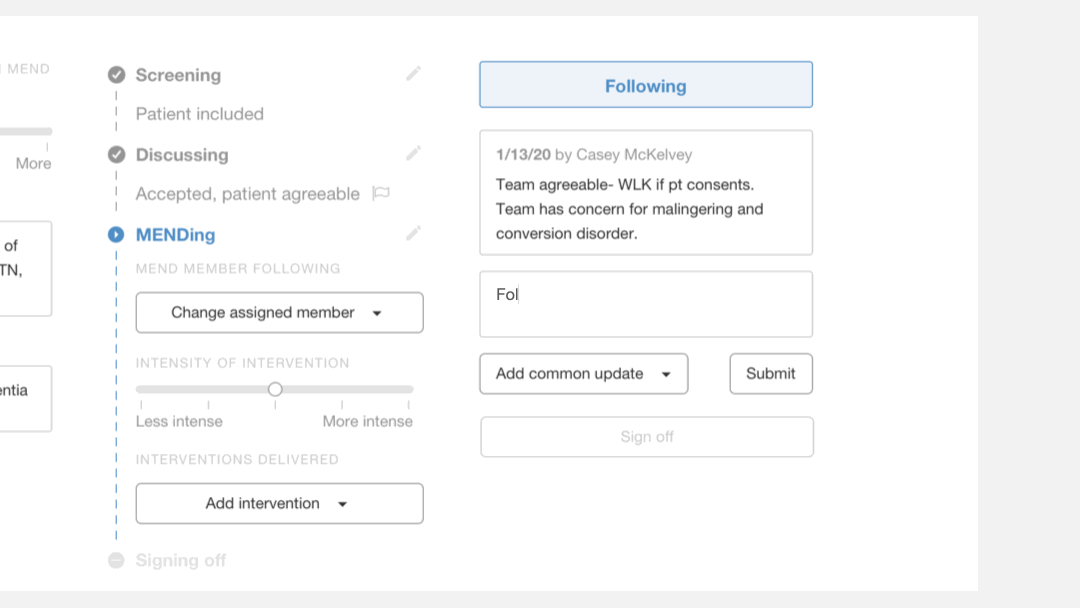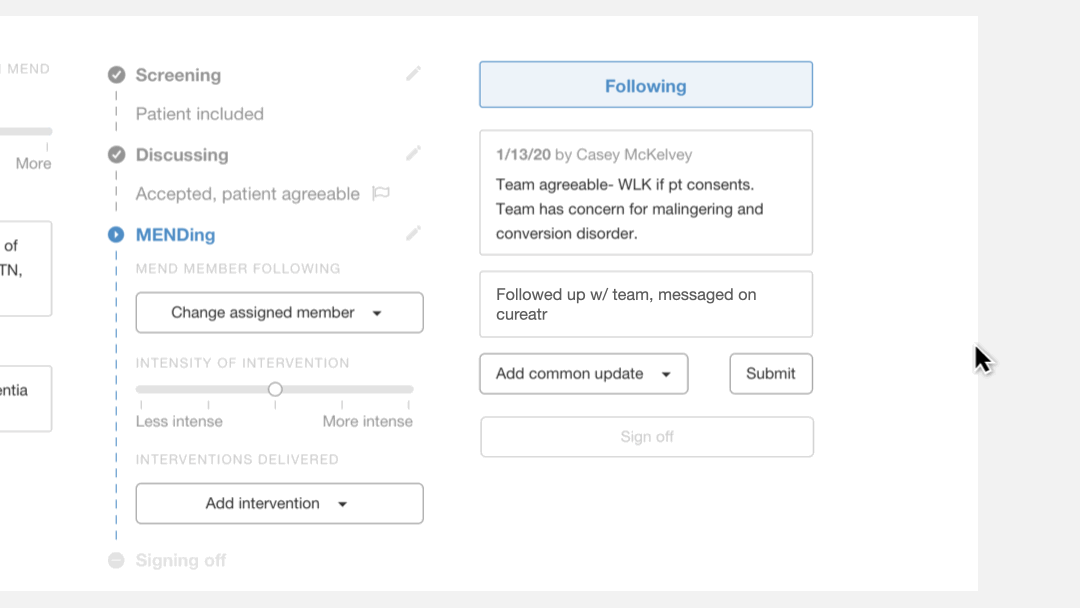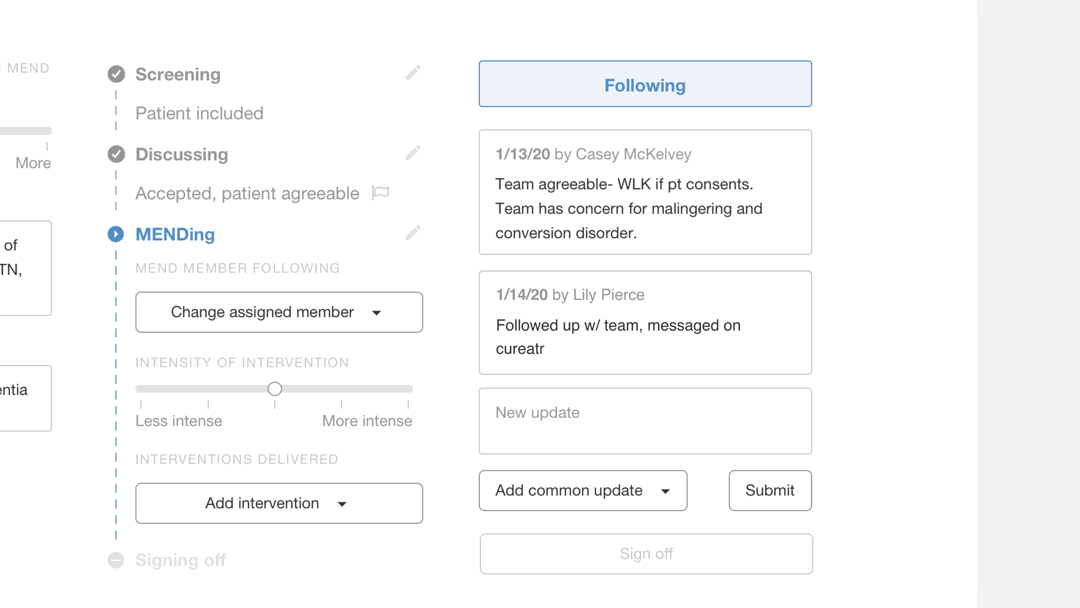
New interaction of documenting an update using the new "Updates" section
Replacing the “Notes” text box, the new “Updates” section is a place where providers submit entries that are displayed in a chronological order with timestamps and names of responsible providers.
In the earlier iterations, clinical info, which was at the top of the old “Notes” section, was included in this “Updates” section. In later iterations, it is moved towards the second column, as writing it is usually one of the first things providers do when they begin a patient case.
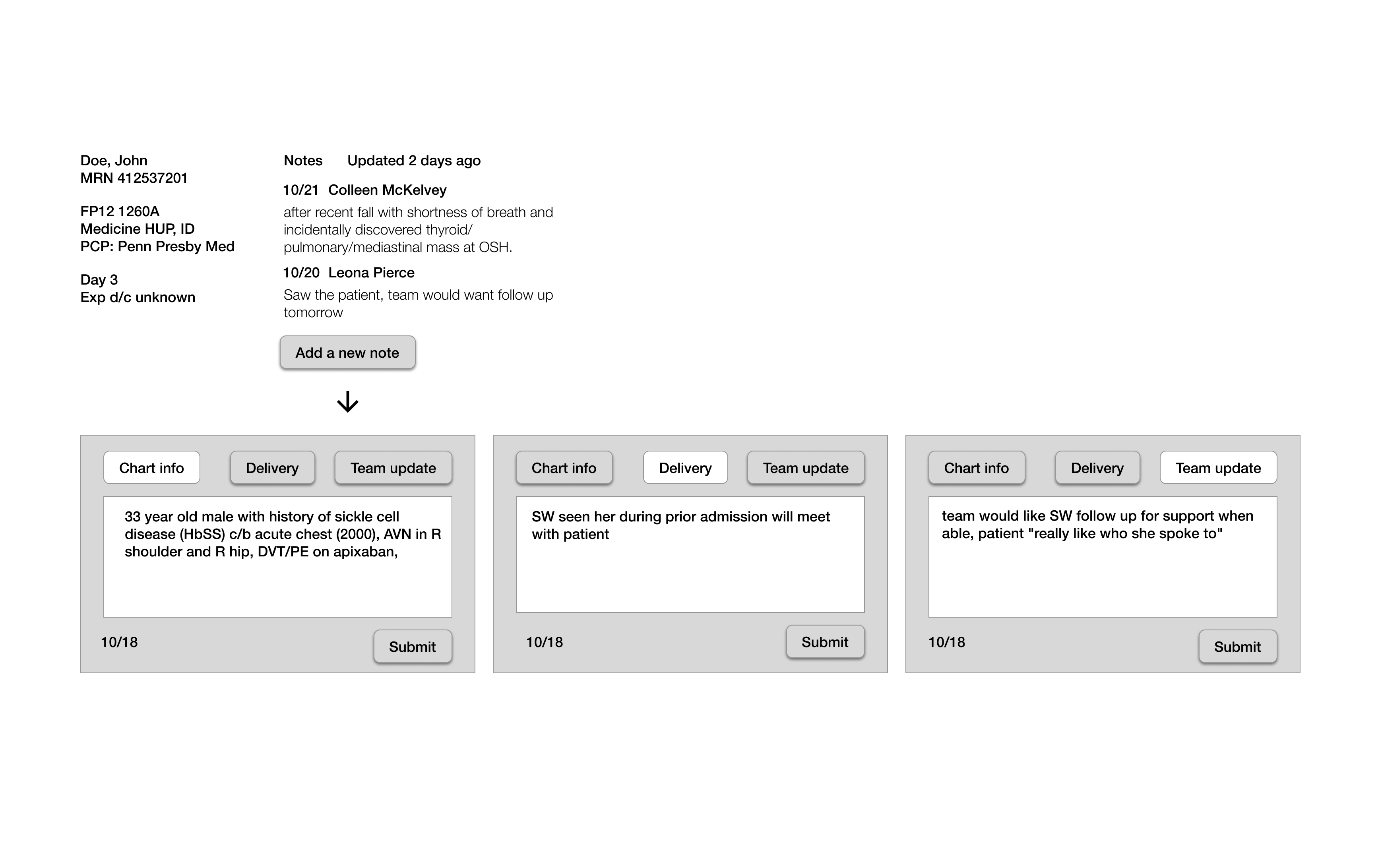
Early lo-fi wireframes of the "Updates" feature
Desired outcome
By creating this section, I hypothesize that providers will be able to glance through updates about patient cases more efficiently, without missing any important information. The time saved would be applied to more clinical time with patients, which the providers valued more. Having their names shown would also increase their sense of ownership.
Impact
I'm currently in touch with my old project team to see if there has been a quantitative impact including decrease percentage of undocumented patient cases, and am scheduling follow-up interviews with users to evaluate qualitative impact.
Reflection
It is truly fulfilling seeing my designs implemented and having a positive effect on real people - improving providers’ workflow and the delivery of healthcare to patients.
My biggest takeaway from this project is the importance of establishing baseline data. There are some baseline data of this project missing, making it hard to test some of my design assumptions. For example, because I didn't test the average time it take to document data per patient case or per day, I couldn't know if the new design really decreased the time users spent.

Resume
© 2021 Mike Dong